The role of the plantaris tendon in Achilles pain.
Published on
05 Sep 2016

Call us on: (03) 9975 4133
Not all Achilles pain is created equal. Ben Westaway talks diagnosing pain in the busy intersection between heel and foot.
A common problem.
The Achilles heel: it’s a common complaint from patients across all activity levels, ages and body types.
There are several causes of pain in the area spanning from the bottom back of the heel, up to the Achilles’ tendon and calf muscle complex.
Due to the complexity of the area, it’s important to thoroughly assess and identify the exact source of discomfort. Different presentations of Achilles pain may require individually tailored treatment solutions.
At Pure Physio, we see from experience that putting a specific treatment plan in place is the most effective factor driving a speedy recovery.
A look at the Achilles.
In this article, we look at one particular type of Achilles pain. This type is generalised to the Achilles’ tendon – and is felt a little higher on the foot.
The pain is felt between 6 and 8 cm above the base of the heel; higher than ‘textbook’ mid portion Achilles pain. The pain tends to concentrate to the medial (inside) aspect of the Achilles’ tendon.
This site is a crossroad of structures in the calf/Achilles complex.
The tendon of the Plantaris muscle joins with the Achilles’ tendon at this merge site.
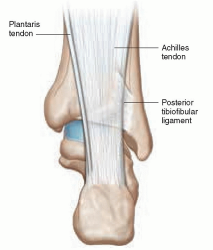
The Achilles tendon from the back of the heel and foot.
Much like a busy traffic intersection, this can be a site of complications.
The plantaris tendon can place undue force on the medial Achilles – reducing its ability to do its job effectively. This condition is called tendinopathy.
The role of the plantaris in tendinopathy presents similar symptoms to true Achilles’ tendon pain.
The area often feels stiff, especially after periods of rest. The first steps out of bed in the morning are often the most troublesome. However, the pain gets progressively less severe as the tendon ‘warms up’ through movement.
While this subset of Achilles pain looks, and feels, similar to ‘textbook’ midportion tendon pain – a correct diagnosis is essential. It’s important to identify whether the plantaris is a contributing factor to discomfort, as this identification may create changes in the approach to treatment.
This distinction could mean the difference between continued discomfort and a successful recovery.
When anatomy collides.
Due to the anatomy of where the plantaris and Achilles’ tendons meet, there are two particular movements of the foot that can contribute to increased pain. These are ankle dorsiflexion, and foot pronation.
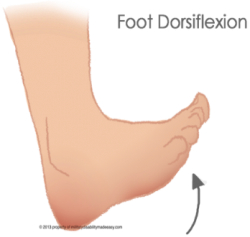
Ankle, or foot dorsiflexion is the action of lifting the toes toward the shin
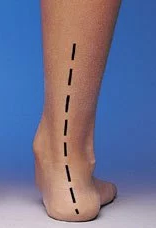
Foot pronation is the inward rolling of the foot and flattening of the arch.
A carefully constructed rehab exercise program that considers these things is paramount to success. For example, unlike genuine midportion Achilles pain, plantaris-involved tendinopathy treatments may discourage heel raises off a step. This exercise may increase symptoms as the ankle forms dorsiflexion.
Find the perfect fit.
Choosing the correct footwear is all part of the healing process. Shoes that are suitable for your individual biomechanics can decrease the loading on this tendon junction.
A podiatry assessment is a great place to find out which shoes are most suited to your foot and lower limb mechanics. Patients with plantaris related Achilles pain generally do worse in flat shoes – so a small heel can be a useful tool in offloading stress and pain.
Getting fitted for an orthotic can also help with symptom management. An orthotic is a valuable clinical tool which is placed inside the shoe to address painful foot and leg movements.
In summary: stay moving.
Achilles pain is extremely common, and can affect anyone. Due to its varying causes, assessing the source of pain is critical for a correct diagnosis and effective recovery process.
By learning the individual risk factors that contribute to your pain, we can develop and implement an individual treatment and rehab plan.
This may involve orthotics, modifying your footwear or a combination of stretching, remedial massage and specific rehabilitation exercises.
Following recovery, incorporating physio exercises can aid in combating recurring pain or injury – it’s important to stay on the move!
If you’re experiencing any pain in the heel or foot, or you’d like assessment and recommendations, get in touch with the team to see how we can help.


